Built for ENT
For an ENT Practice,
Blue Does It.
Blue processes your fax referrals, contacts your patients, schedules your appointments, and generates your prior auth paperwork. Not as a tool your staff uses. As work that gets done automatically.
0+
Patients Triaged
0+
Fax Pages Processed
0%
Schedule Rate
Daily
Use at ENT Practices
You're spending your day on work
that agents should be doing.
Doctors, nurses, and office staff are all stuck doing work a machine should be doing. Referrals pile up at the front desk. Patients never get scheduled. Documentation and admin tasks eat into time that can be spent on care.
Referrals pile up
Staff reads through 10 to 15 page faxes one at a time looking for patient name, diagnosis, and insurance. At 100+ referrals a day, the pile never shrinks.
Patients don't get scheduled
Phone tag, voicemails, unanswered website inquiries. Patients who want to book just give up. That's $200 to $350 per missed consult.
Documentation and admin eat the day
Doctors write their own notes. Prior auth paperwork piles up. Appeal letters get pushed to tomorrow. Referral correspondence never gets sent. Every one of these is a task that should be happening on its own.
Blue does the operational work that
should be done automatically.
Blue is the AI operations team for your ENT practice. It processes your referrals, contacts your patients, books your appointments, and handles your prior authorizations. Work that used to sit in separate silos across separate people just happens automatically.
Referral Intake
Blue reads your faxes, pulls the data, and
routes every referral to the right team.
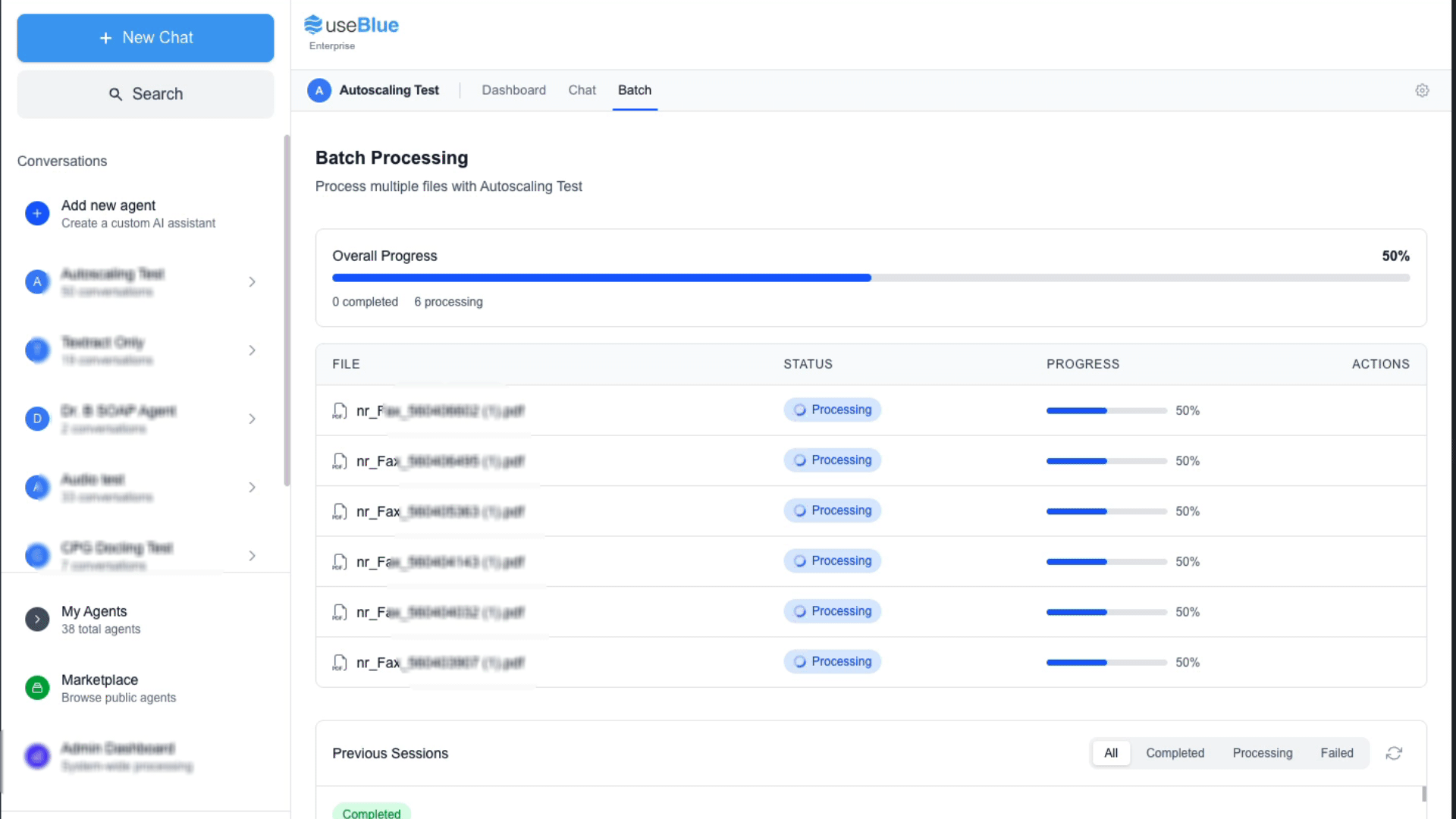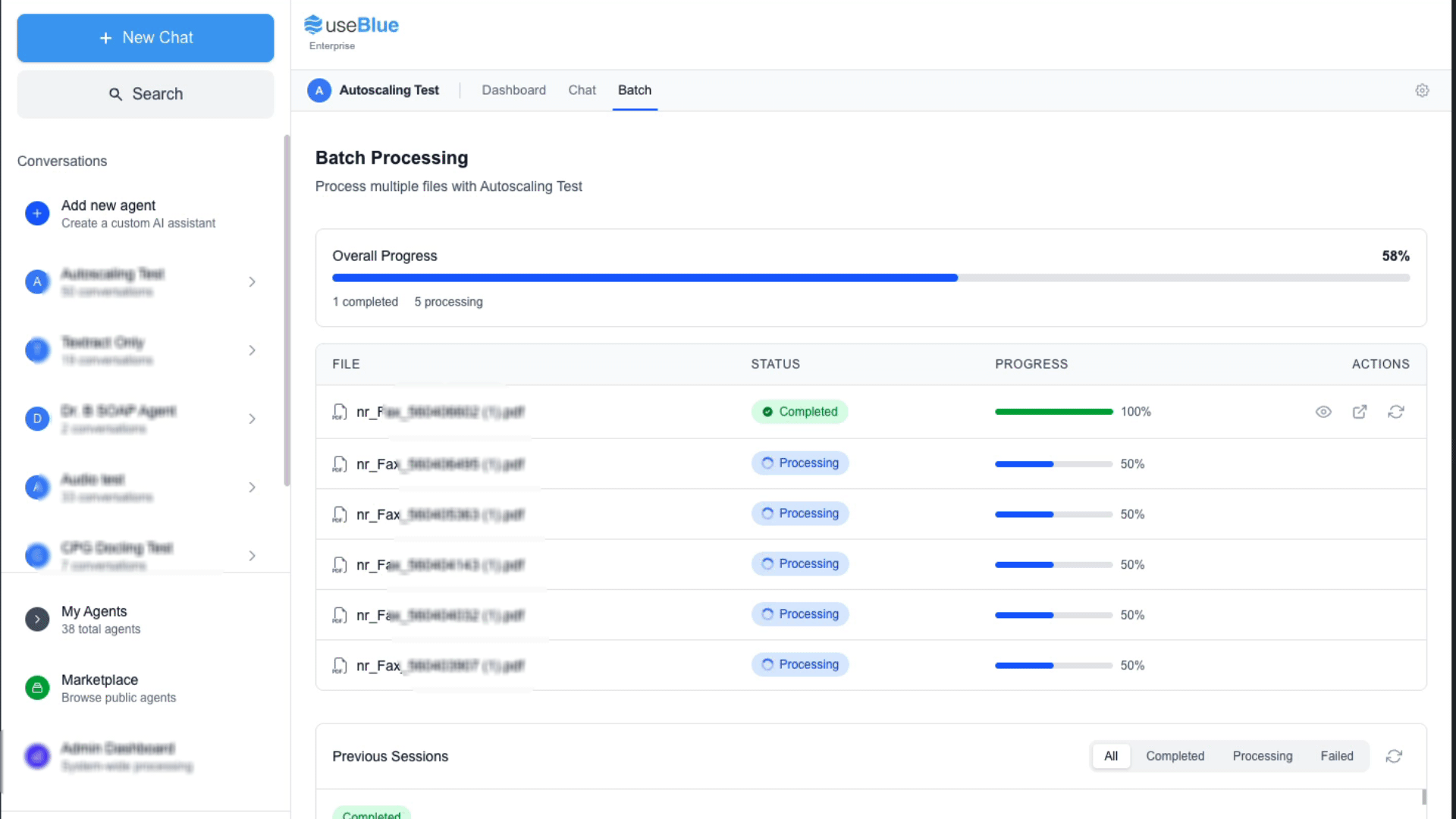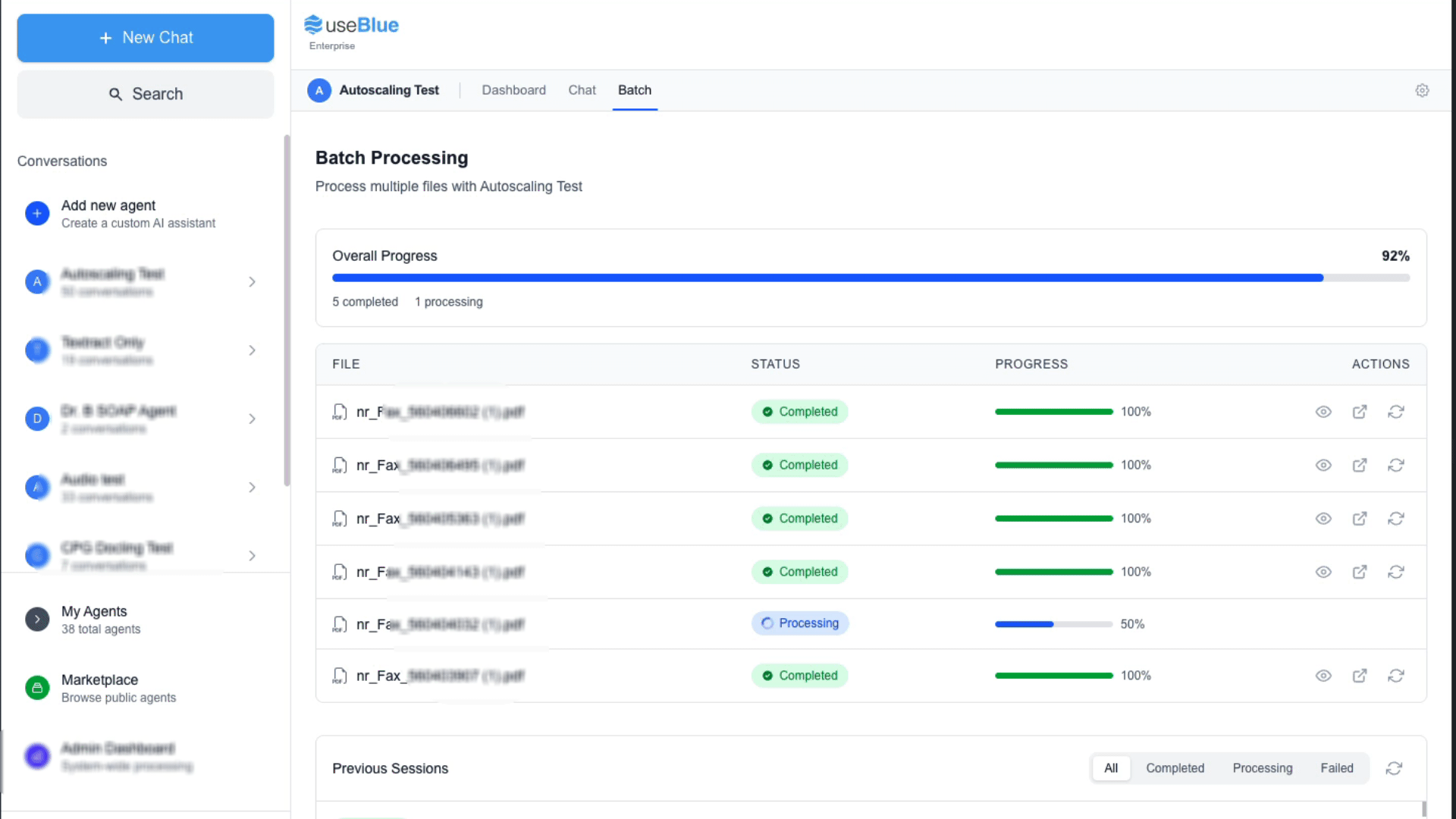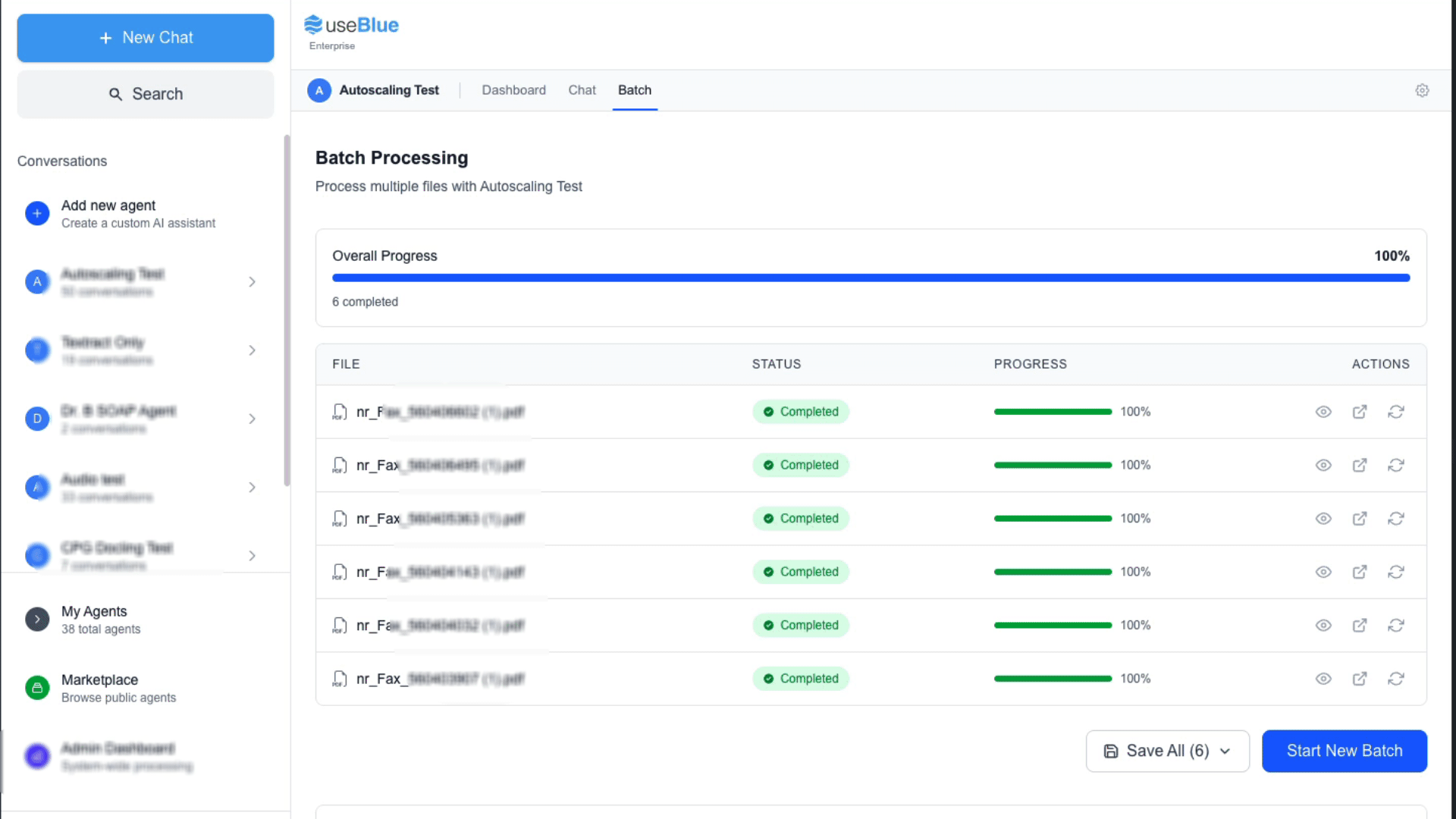
A fax arrives. Blue opens it, reads every page, and extracts the patient's name, date of birth, diagnosis, insurance, referring provider, and urgency level. Then it routes the referral to the right provider or department based on rules you set.
What Blue does:
- Ingests faxes from Ring Central, eFax, SRFax, or any email-based fax system
- Extracts structured patient data from documents of any length
- Routes by diagnosis, urgency, insurance, location, or any extracted field
- Notifies the right team with a secure platform link (no PHI over email)
Patient Engagement and Scheduling
Blue contacts your patients, qualifies them,
and gets them on the schedule.
Once a referral is processed, Blue texts the patient with a personalized message and a link to self-schedule. For website visitors, Blue runs quiz agents that capture symptoms, qualify the patient, and trigger outreach automatically.
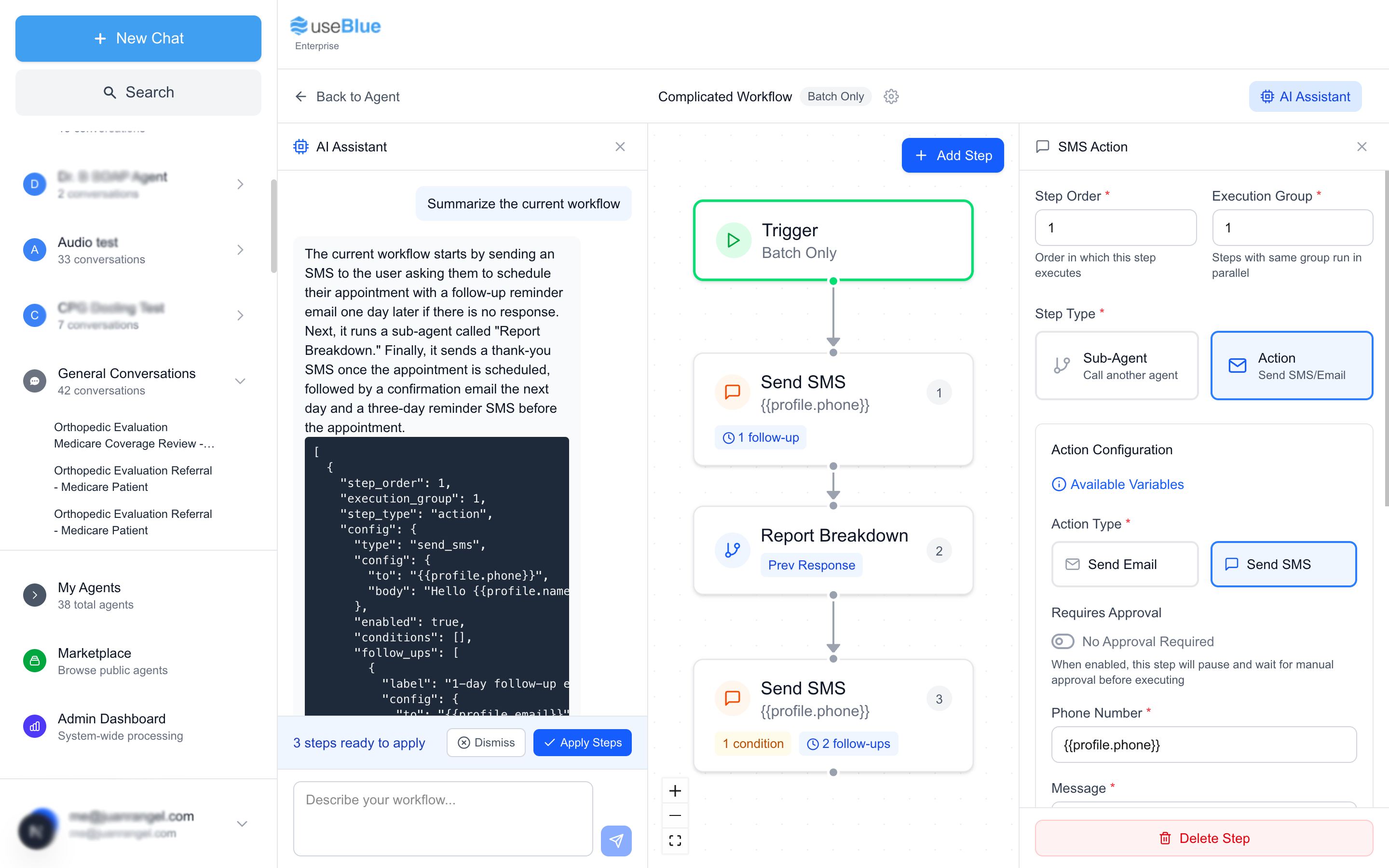
What Blue does:
- Sends HIPAA-compliant SMS with self-scheduling links
- Runs follow-up sequences automatically (not just one text)
- Embeds symptom quiz agents on your website (sinus, sleep, and custom)
- Integrates with ZocDoc or your direct booking system
- Tracks every patient: contacted, responded, scheduled, no-show
Prior Authorization Automation
Blue writes the prior auth paperwork while
you're still talking to the patient.
Prior auth is one of the most painful admin tasks in ENT. A CT gets denied. An appeal takes hours. A surgery gets delayed. Blue listens to the visit context, catches the payer the moment it's mentioned, and automatically generates authorization documentation formatted to that payer's specific requirements.
I was reviewing a patient's CT and giving her my standard insurance authorization talk. I mentioned United Healthcare as her carrier. I didn't think twice about it. After the visit, two extra notes showed up in my email: documentation formatted specifically for United's requirements to get the CT approved. The system caught the payer context from the conversation and generated the paperwork I would have needed to do later, or hand off to billing, or honestly just not get to that day.
That's not a prior auth tool. That's the prior auth getting done.
What Blue does:
- Detects the payer automatically from visit context
- Generates payer-specific authorization documentation in real time
- Formats notes to meet medical necessity requirements for each carrier
- Delivers finished paperwork to the right person before the patient leaves
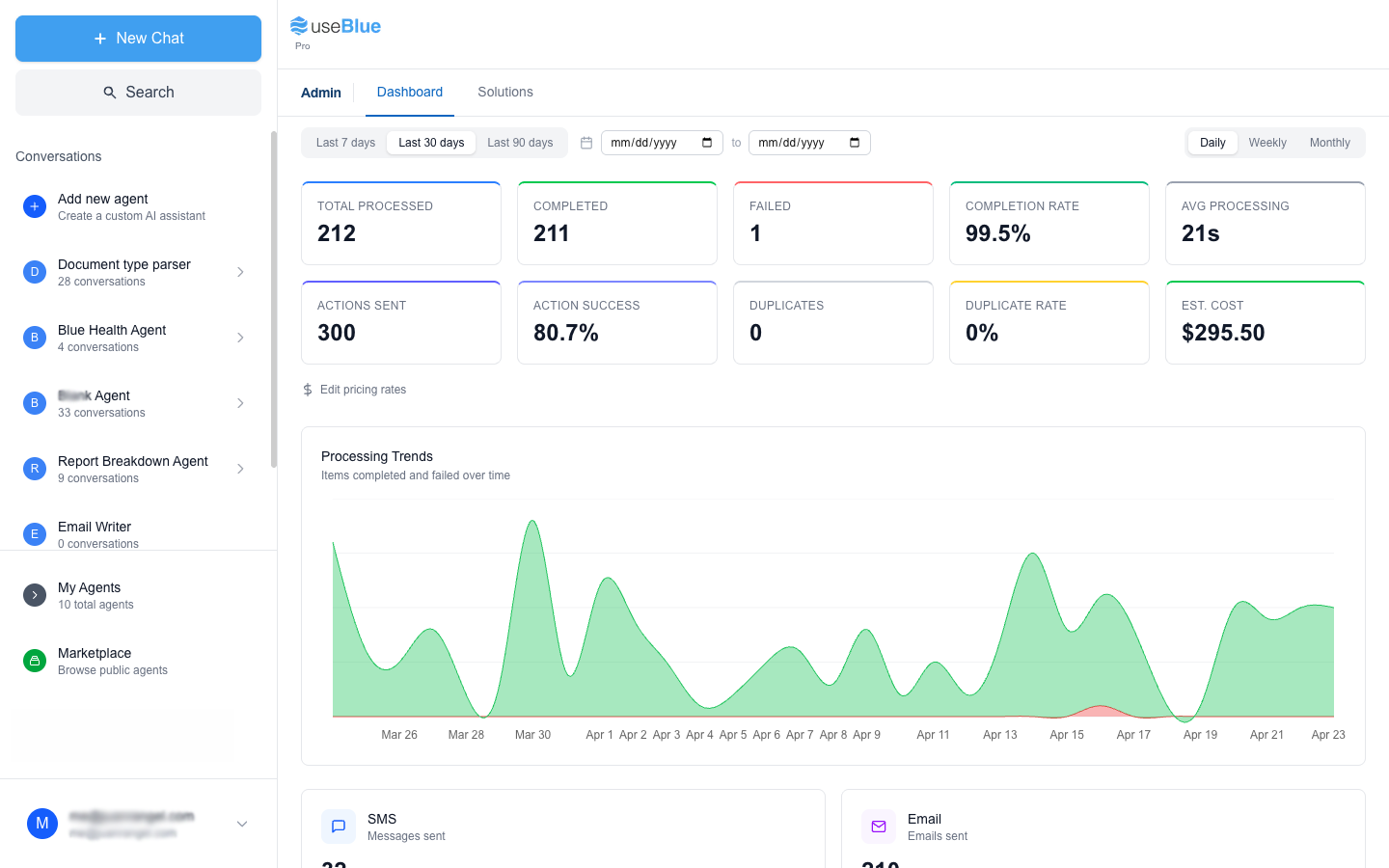
Ready to Automate Your ENT Practice?
Most healthcare software needs a team to run it. For every $1 you spend on the tool, you spend $6 on the people managing it. Blue was built to end that.
No long-term contracts. Free plan available. BAA included.